- The purposes of ultrasound-guided prostate
biopsy are to confirm the diagnosis, assess treatment efficacy, and evaluate
disease progression.
- Prostate biopsy can be performed via transrectal
or perineal approaches.
- Post-procedural care following ultrasound-guided prostate biopsy includes monitoring for hematuria, abstaining
from sexual activity for two weeks, and avoiding heavy lifting for one month.
According to statistics released by the Ministry of Health and Welfare in 2024, Among the ten leading causes of death in Taiwan, prostate cancer ranks fifth. With early diagnosis and effective treatments, the five-year survival rate can exceed 75%.
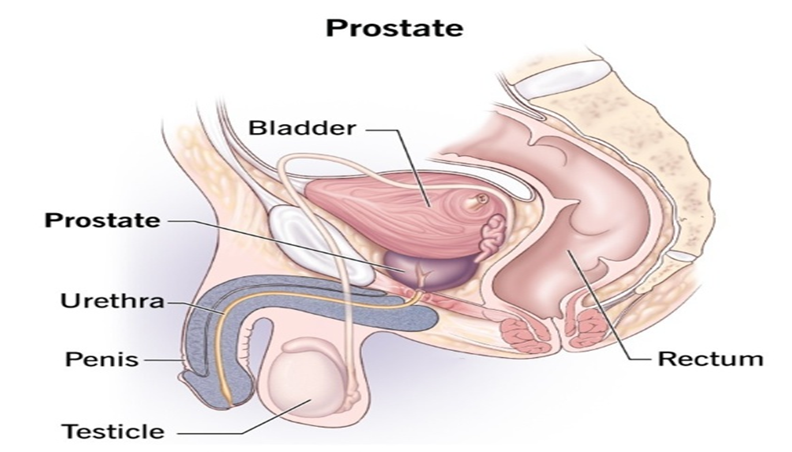
The prostate is a glandular
organ that resembles a chestnut in shape, weightss about 20 grams, and secretes
prostate fluid, which is a component of semen. It is located below the bladder,
surrounding part of the urethra, and is separated from the rectum by a fascial
layer (Figure 1).
II.Why Undergo Ultrasound-Guided Prostate Biopsy
Early-stage prostate cancer typically presents without symptoms. Currently, diagnosis involves a physician performing a digital rectal examination (DRE) and measuring blood levels of prostate-specific antigen (PSA). Additionally, depending on the clinical situation, the physician may consider newer diagnostic tests such as the Prostate Health Index (PHI) or magnetic resonance imaging (MRI) at the patient's expense. Based on the combined results of these examinations, a prostate biopsy under ultrasound guidance is performed to confirm the pathological diagnosis, Purpose:
- To differentiate between various prostate
pathologies.
- To stage and diagnose prostate carcinoma.
- To evaluate the therapeutic efficacy of radiation or hormone therapy in prostate cancer management.
- To actively monitor the progression of untreated
prostate carcinoma.
III.Examination Methods
The physician conducts an ultrasound scan by inserting a lubricated transducer probe either into the perineal area or 2-4 centimeters into the rectum. When required, a prostate biopsy is performed under ultrasound guidance. For MRI-ultrasound fusion-guided biopsy, pre-acquired MRI images are fused with real-time ultrasound images to accurately plan and target the biopsy sites. The entire procedure typically takes approximately 30-60 minutes.
- Examination Methods
- Transrectal Ultrasound-Guided Prostate Biopsy (TRUS).
-
Transperineal Ultrasound-Guided Prostate Biopsy
-
MRI-Ultrasound Fusion-Guided Prostate Biopsy
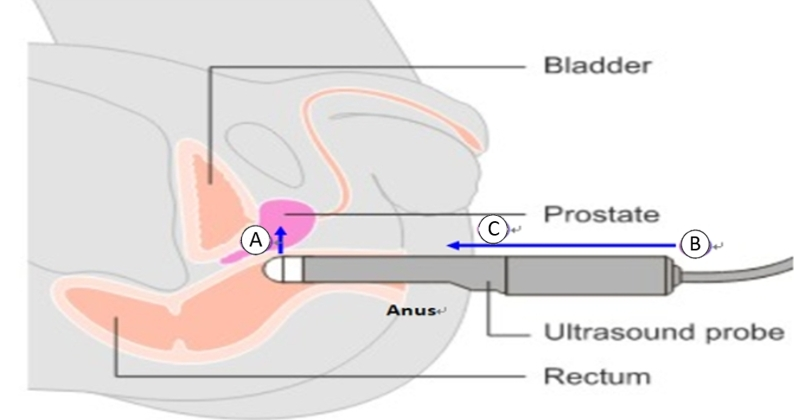 (Image source: Generated by AI)
(Image source: Generated by AI)
-
Before the Examination
-
Complete the ultrasound-guided prostate biopsy information and consent form, as well as the surgical and anesthesia consent forms.

(Image source: Generated by AI) -
Administer prophylactic antibiotics as prescribed by the physician.

(Image source: Generated by AI) - The nurse administers a morning enema per the physician's instructions to ensure thorough bowel preparation.
(Image source: Generated by AI) - For MRI-ultrasound fusion-guided biopsy, a magnetic resonance imaging (MRI) scan must be performed beforehand.
(Image source: Generated by AI)
-
Complete the ultrasound-guided prostate biopsy information and consent form, as well as the surgical and anesthesia consent forms.
- During the Examination: The examination and positioning method will be selected based on the physician's clinical evaluation. The following two approaches are available
- Transrectal Approach: The patient is positioned in the lateral decubitus position with the knees drawn up (flexed).

(Image source: Generated by AI) - Transrectal or Transperineal Approach: The patient is positioned in the supine lithotomy position.
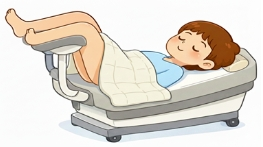
(Image source: Generated by AI)
- After the Examination
- Occasional hematuria, rectal bleeding, and hematospermia may occur, typically resolving within 1-2 weeks.

(Image source: Generated by AI) - Acute urinary retention may occur, requiring catheterization based on clinical assessment.

(Image source: Generated by AI) - Maintain a daily fluid intake of 3000 mL.

(Image source: Generated by AI) - Abstain from sexual intercourse and avoid warm sitz baths for two weeks.

(Image source: Generated by AI) - Administer antibiotics as prescribed by the physician and avoid discontinuing the medication to prevent inflammation.

(Image source: Generated by AI) - Per physician’s instructions, avoid heavy lifting or strenuous activities such as sit-ups, cycling, swimming, and running for one month post-procedure.

(Image source: Generated by AI) - Follow the physician's instructions for scheduled follow-up visits. If symptoms such as chills, fever, severe hematuria, difficulty urinating, or persistent rectal bleeding occur, seek medical attention immediately
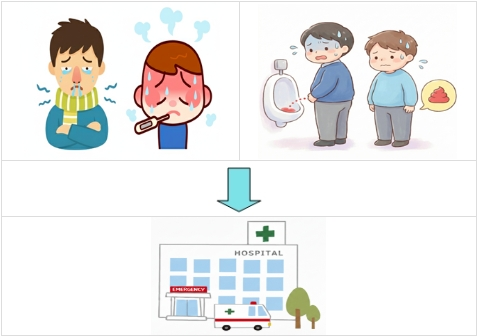
(Image source: Generated by AI)
IV.Conclusion
Patients undergo a digital
rectal examination (DRE) and measurement of prostate-specific antigen (PSA)
levels in the blood during outpatient visits. Combined with other assessments
such as the Prostate Health Index (PHI) or magnetic resonance imaging (MRI), if
abnormalities are detected, the physician will evaluate and schedule an
ultrasound-guided prostate biopsy to confirm the pathological diagnosis. This
assists the physician in clinical judgment and planning subsequent treatment.
VI.References
- 王賢祥(2024,1月12日)。攝護腺癌診斷的利器-經直腸超音波攝護腺切片。https://www.vghtc.gov.tw/UnitPage/RowViewDetail?WebRowsID=57887c2b-b74b-447b-8fb2-c7d1e29134df&UnitID=b8390b70-75ec-4335-b22c-ce217ddcaad2&CompanyID=e8e0488e-54a0-44bf-b10c-d029c423f6e7&UnitDefaultTemplate=1
- 廖博崎(2024年1月12日)。磁振造影融合影像機械手臂超音波引導經會陰攝護腺切片。https://www.vghtc.gov.tw/UnitPage/RowViewDetail?WebRowsID=cb0a2ca6-1b75-4c4b-90b3-dd8e434080ae&UnitID=b8390b70-75ec-4335-b22c-ce217ddcaad2&CompanyID=e8e0488e-54a0-44bf-b10c-d029c423f6e7&UnitDefaultTemplate=1
- Chen, Y., Wang, Y., Wang, J., Rao, M., Li, C., Wang, Y., & Huang, Y. (2025). Clinical study on mpMRI/TRUS software fusion-guided transperineal prostate biopsy. Journal of Men’s Health, 21(1), 81–86. https://doi.org/10.22514/jomh.2025.008
- EAU guideline(2025).Prostate cancer. https://uroweb.org/guideline/prostate-cancer/
- Wu, T. & Xing, Y. (2024). Ultrasound-guided transperineal vs transrectal prostate biopsy: A meta-analysis of diagnostic accuracy and complication rates. Open Medicine, 19(1), 20241039. https://doi.org/10.1515/med-2024-1039
- 位置
-
- 資料夾名稱
- English
- 上傳者
- 紀妍菲
- 單位
- 中榮護理衛教
- 英文名稱
- Information on Ultrasound-Guided Prostate Biopsy
- 分類
- 檢查
- 科別
- 英語
- 癌症照護
- 否
- 建立
- 2024-06-21 12:43:32
- 最近修訂
- 2026-03-17 17:50:34
- 版本
- 2026-03-17